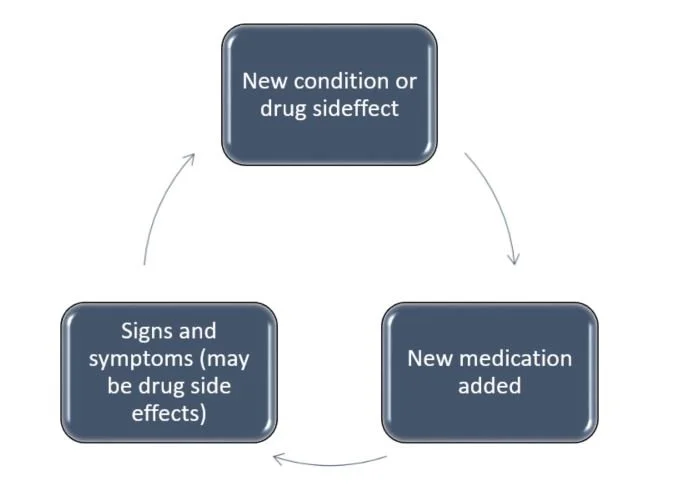
When Side Effects Turn Into New Diagnoses
The Prescribing Cascade: When the Fix Becomes the Problem
You feel dizzy. So a new medication is prescribed.
Then you fall. So another medication is added.
Then you’re confused. So now we’re treating memory loss.
This is called a prescribing cascade — and it happens every single day.
A prescribing cascade occurs when a side effect from one medication is mistaken for a new medical condition, and another drug is prescribed to treat it.
Common examples I see as a pharmacist:
A blood pressure medication → swelling → diuretic added
A bladder medication → confusion → memory medication added
A pain medication → constipation → laxatives added
A sleep medication → morning grogginess → stimulant added
Before long, the medication list doubles — and no one paused to look upstream. Too Many Meds? Time to Reconcile!
What Often Gets Missed
We rarely go back to the beginning.
Why was the original medication started? Is it still necessary? Is it the right drug for this person at this stage of life?
Could a different medication — or a lower dose — accomplish the same goal with fewer side effects?
Sometimes the better move isn’t adding something new, it’s adjusting what came first.
Give the Drug a Chance
There’s another issue I see frequently.
Many medications need time to reach a therapeutic level. Early side effects can lessen as the body adjusts. But patients understandably get uncomfortable. They call within days.
A second medication is added before the first one has even had a fair chance to work.
Now we’re layering drugs unnecessarily.
And once they’re added? They tend to stay.
That’s how polypharmacy quietly builds.
The Good News? Cascades Can Often Be Reversed.
Two important tools help unwind this pattern.
Comprehensive Medication Reviews (CMRs)
A structured, pharmacist-led review of every prescription, over-the-counter product, and supplement. We look at interactions, duplications, dosing, and — most importantly — whether each medication still matches the health goal. Polypharmacy & Basic Medical Review
Deprescribing
Not abrupt stopping. Not reckless cutting.
Thoughtful, supervised reduction of medications that may no longer be necessary or beneficial.
Deprescribing asks:
Is this still indicated?
Is the dose appropriate for this age?
Was this added to treat a side effect?
Are risks now outweighing benefits?
When done carefully, reducing medication burden can improve clarity, stability, and quality of life.
Medication safety isn’t about taking nothing. Taking mutiple medicines safely
It’s about taking what’s appropriate — and only what’s appropriate.
If something feels off, or the medication list keeps growing without clear review, pause before adding again.
👉 Ask the Advocate — A second set of eyes today can prevent a cascade tomorrow.
✨ Stay confident. Stay informed. Stay Taylormade.
Cheers!
Dr. T